Robotic & Laparoscopic surgery
Patient Information
This information is for patients considering having an operation where the surgeons will be using the Da Vinci robot.
Introduction
There are a range of surgical procedures that surgeons are able to carry out with the assistance of the Da Vinci robot.
Having an operation using the Da Vinci Robot
How it works
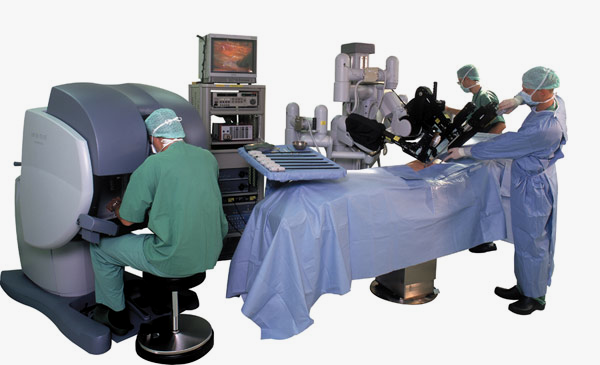
The Da Vinci robot is in the operating theatre alongside the patient. It consists of a surgeon’s console and the robot itself which has four interactive robotic arms controlled from the console. Three of the arms are for surgical instruments. The fourth arm is for an endoscopic camera with two lenses that gives the surgeon full stereoscopic vision from the console. The surgeon sits at the console and looks through two eye holes at a 3-D image of the procedure, meanwhile manoeuvring the arms with two foot pedals and two hand controllers. The Da Vinci robot system translates the surgeon’s hand movements into more precise micro-movements of the instruments, which operate through small incisions in the body.
Throughout the operation the surgeon is always in charge. The robot is a ‘slave’ and will only do what the surgeon instructs it to do. It is a helper that holds the instruments and can keep completely steady at all times, making the most delicate of movements. This means that very great accuracy can be achieved during operations and that the surgeon can clearly see what needs to be done inside the patient’s body.
The benefits of robotic-assisted surgery
The main benefits to patients are that the surgery can be carried out with minimally-invasive techniques. Operations are carried out with the patient asleep under a general anaesthetic. Using incisions in the body – known as ‘ports’, instruments can be inserted and moved to exactly where they are needed. A small camera is also inserted through one of the ‘ports’ so that the surgeon can see the parts to be operated on and manoeuvre the different instruments.
Robotic surgery is still a ‘major’ operation with risks and benefits to take into consideration when deciding what is best for a particular patient. However, operations that once involved large incisions and lots of stitches can now be carried out with robotic assistance. This means that recovery time for the patient is comparatively much shorter. They are less sore afterwards and can resume their normal life more quickly.
Am I suitable for robotic-assisted surgery?
The range of procedures that can be carried out with robotic assistance is being extended as time goes on. Your consultant surgeon will discuss with you whether you would be a suitable patient for robotic surgery and also tell you what the alternatives, risks and benefits of surgery would be.
If robotic-assisted surgery has already been discussed with you and agreed as the preferred option more information about preparing for your operation, coming into hospital and care at home afterwards will be given to you.
Robotic Ventral Mesh Rectopexy Operation
Patient Information
What is a robotic ventral mesh rectopexy?
The term ‘rectopexy’ refers to an operation in which the rectum is suspended back into its normal anatomical position by the use of a supportive mesh. If appropriate the bladder and, in women, the vagina may also be re-aligned at the same time. Robotic rectopexy is the term used when the surgeon is assisted by the Da Vinci surgical robot during the operation.
When is rectopexy performed?
One of the most common reasons for performing the procedure is for patients with external rectal prolapse (bowel coming out through the anus) or internal prolapse or “intussusception” when the rectum prolapses internally within the rectum, without coming out of the anus. This may cause obstructed defaecation syndrome (ODS). These patients commonly have a sensation of a blockage of the bowel, difficulty in passing a motion, prolonged (often unsuccessful) visits to the toilet and a frequent need to apply pressure with a finger or hand on the perineum, in the vagina or the anus to empty the bowels. Internal rectal prolapse sometimes causes faecal incontinence and robotic rectopexy may help these patients.
What tests are necessary before the operation?
Your consultant will see you in the outpatient clinic to assess your symptoms and to perform an initial examination. There is a range of tests available to help your consultant arrive at the most appropriate course of treatment and patients will have one or more of these. The tests could include an endoscopic (telescope) test on the bowel; physical examination of your anus; an ultrasound; or an MRI proctogram which involves inserting gel into the rectum which is expelled whilst MRI images are taken to see how well supported your pelvic organs are during the process of emptying your bowels. These tests are carried out as outpatient procedures. You may also have a consultation with a physiotherapist who specialises in helping patients who have difficulty emptying their bowels.
What does the operation involve?
The operation is performed under general anaesthetic by keyhole surgery and with the assistance of the Da Vinci robot. It takes three to four hours. You will be asked to come to the hospital early on the morning of your operation. Approximately an hour before the procedure, a nurse will give you an enema to empty your rectum prior to surgery.
The surgery is carried out through your stomach (not up your bottom). It usually involves a small cut just above the umbilicus (belly button) and four to five other small cuts on the tummy. A camera and instruments are then inserted through these ‘ports’ into the tummy. With the clear view given by the camera, the surgeon creates a space as far down as possible between the rectum and vagina. A non-absorbable mesh is then stitched to the front of the rectum and back of the vagina and then fixed to the sacrum or lower part of the backbone.
The operation pulls the bowel out of the pelvis, restoring it to its normal anatomical position and prevents it from telescoping back down into the pelvis. The position of the lower end of the mesh between rectum and vagina supports the rectovaginal septum (the thin structure between the rectum and vagina) and corrects any rectocele (bulge from the rectum into the vagina) and enterocele (small bowel dropping into the pelvis between vagina and rectum). When the operation is over you will be admitted to a hospital ward where you will usually stay overnight and be able to go home the day after your operation.
How do I prepare for having my operation?
A week or two before your operation date you will be asked to come to hospital for ‘pre-assessment.’ At this outpatient clinic you will have some tests, such as a blood test and ECG (test of your heart rate and rhythm) to make sure you are fit enough to have an operation. You should generally aim to make any lifestyle changes that will help you during and after your operation. For example stopping smoking, reducing alcohol intake and improving your diet can help you get the best possible outcome in the long term.
What is the recovery like after surgery?
The main benefit of robotic-assisted rectopexy is that the operation is done with a minimum of disturbance to the skin and muscles of your tummy. Your anaesthetist will discuss pain control with you before the operation and will use a long-acting anaesthetic during the surgery that will gradually wear off over the next 12 hours or so. You will wake up from the operation with a catheter (tube) in your bladder so that you do not need to get up to use the toilet and a drip in your arm to make sure you do not get dehydrated. On the morning after surgery, your catheter will be taken out and your drip will usually be finished. You will be able to eat and drink and all being well, should be able to go home later in the day. Patients usually stay in hospital for one or two nights but may occasionally need to stay longer.
You will be discharged on a course of laxatives and you should take these for six weeks. It is important you do not get constipated and strain in the first few weeks after surgery as this causes pain. Occasionally patients may become constipated as a result of pain relieving medication. If you become constipated, you should seek advice from your doctor. Do not delay seeking help with symptoms of constipation. In order to get the best possible outcome, make sure that your diet is well-balanced in the long term. Your surgeon will usually see you in his outpatient clinic six weeks after your operation.
You may be fit to drive after a week, return to work after two weeks but should not do any lifting for at least six weeks.
What are the results like from surgery?
For patients with external prolapse, the operation has a very low rate of recurrence (i.e. the prolapse coming back), around 5%.
Suitable patients with internal prolapse can also expect good results from surgery. For patients with obstructed defaecation, the majority of patients will have a significant improvement in their symptoms. There may also be an improvement in continence.
However, it is difficult to predict those patients who do not benefit from surgery. For these patients, other additional measures can be helpful.
What are the risks of surgery?
This is relatively low risk surgery. Older versions of rectopexy involved removing segments of bowel and making joins that increased the risks of the operation. Bowel was removed to offset the worsening of constipation that rectopexy would often cause as a consequence of nerve damage. With robotic rectopexy, the nerves are avoided and constipation rarely gets worse. There are small risks such as bleeding and infection or the need to proceed to an ‘open’ surgical procedure during the operation. There have been a few cases reported of mesh-related problems but the risk of these is small.
Is robotic ventral mesh rectopexy better than other prolapse operations?
As a laparoscopic (keyhole) procedure, this operation is more cosmetic and less painful than open surgery (involving large cut down the middle of the tummy). We use mesh as this seems to produce a more long lasting result. Prolapse rarely comes back after laparoscopic rectopexy (around 5%) compared to operations from a perineal (through the anus) approach (over 20%).



